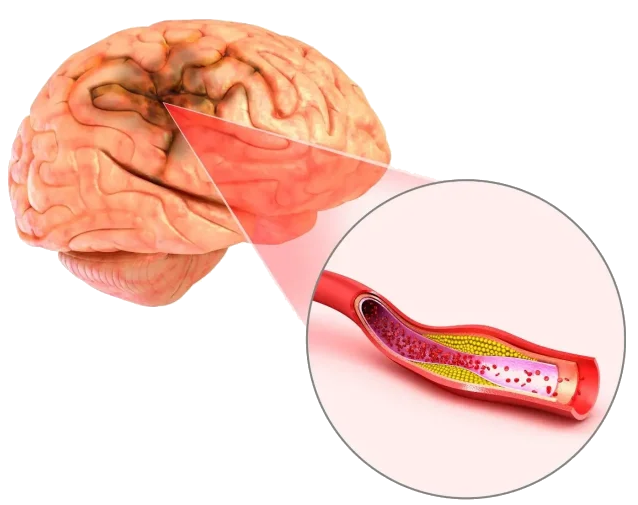
Elevated cholesterol levels, referred to as hyperlipidemia or dyslipidemia, contribute significantly to blood vessel disease, a common precursor to stroke.
Cholesterol, a pliable, fatty substance, is both produced by the body and absorbed from certain foods like eggs, meats, and dairy products. A diet rich in saturated fats, particularly those from animal sources, is the primary culprit behind high cholesterol levels, although genetic factors can also play a role.
Cholesterol exists in two forms:
The ratio of HDL to LDL cholesterol serves as a critical indicator of stroke risk. Higher levels of HDL correspond to a reduced risk, whereas increased LDL levels elevate the risk.
Excessive cholesterol in the bloodstream can lead to atherosclerosis, wherein cholesterol accumulates on artery walls, causing narrowing or blockages. This condition, in turn, can impede blood flow or trigger blood clots, predisposing individuals to ischemic strokes.
Control your risk
Discuss with your healthcare provider your current cholesterol levels and establish goals to mitigate your stroke risk.
To lower cholesterol, dietary adjustments, physical activity, and medication are effective strategies:
If necessary, your doctor may prescribe lipid-lowering medication to manage cholesterol levels, especially following an ischemic stroke.
Various lipid-lowering medications are available, each with distinct mechanisms of action. Some medications specifically target LDL (the “bad” cholesterol), while others address overall cholesterol levels.
Statins are frequently prescribed to lower cholesterol and mitigate stroke risk. Your healthcare provider can recommend the most suitable medication for your needs.